Antibiotics in Livestock
|
Here’s the truth… there are no antibiotics in your food. At all. There are no antibiotics in your milk. There are no antibiotics in your meat. There are no antibiotics in your eggs. Period. However, livestock animals are occasionally treated with antimicrobial medications. A widely spouted statistic is that 70-80% of the antibiotics sold in America are used to treat livestock. However, less than a third of antibiotics used on farm animals are relied on in human medicine.
Why Are Antibiotics Used? At the turn of the century, antibiotics were being taken advantage of because of their outstanding promotion of growth. This was resulting in large numbers of head being at risk of entering the food supply with antibiotics still in their system which was jeopardizing food safety. |
To put a stop to this, in 2013, the FDA outlawed antibiotics for use in growth promotion. To enforce this, regulations were changed so that antibiotics could only be obtained with a prescription from a certified veterinarian who could confirm that the animal was in need. Furthermore, pharmaceutical companies voluntarily joined the fight against antibiotic misuse by removing any mention of growth enhancement on labels. But why not just ban antibiotics completely?
The truth is that raising livestock without the use of antibiotics is an even bigger food safety risk than allowing antimicrobial residues to be present in our food supply. How’s that? Treating sick or injured animals is often only possible with the use of antibiotics. If we allowed health problems to go untreated, infections or diseases could taint the meat or milk, and do a great deal of harm to the consumer. Not to mention the outstanding welfare violations that would arise from leaving ill animals to suffer, untreated. The good news is that, with improved regulations and enforcement, most animals never come into contact with antibiotics. However, just like with people, accidents can happen. A foot can get caught in the fence, rough playing can cause a gouge, or a common cold can cause sickness.
That’s not to say that farmers haven’t taken a stand to cut back on the need for therapeutic uses of antimicrobial medicines in a lot of ways. Some of these include annual (my family actually did twice a year) vaccinations to prevent disease and boost the immune system, improve facility sanitation, avoid stressors, being aware of common diseases and their symptoms, and working in close capacity with veterinarians.
The truth is that raising livestock without the use of antibiotics is an even bigger food safety risk than allowing antimicrobial residues to be present in our food supply. How’s that? Treating sick or injured animals is often only possible with the use of antibiotics. If we allowed health problems to go untreated, infections or diseases could taint the meat or milk, and do a great deal of harm to the consumer. Not to mention the outstanding welfare violations that would arise from leaving ill animals to suffer, untreated. The good news is that, with improved regulations and enforcement, most animals never come into contact with antibiotics. However, just like with people, accidents can happen. A foot can get caught in the fence, rough playing can cause a gouge, or a common cold can cause sickness.
That’s not to say that farmers haven’t taken a stand to cut back on the need for therapeutic uses of antimicrobial medicines in a lot of ways. Some of these include annual (my family actually did twice a year) vaccinations to prevent disease and boost the immune system, improve facility sanitation, avoid stressors, being aware of common diseases and their symptoms, and working in close capacity with veterinarians.
Should You Buy Products Free of Antibiotics?
Farmers take great pride in producing high quality and safe products. Remember that they often keep products for their own families to use. Here’s a statement from one of my favorite blogs, Ask The Farmer’s, article about the needs and risks of antibiotics:
Farmers take great pride in producing high quality and safe products. Remember that they often keep products for their own families to use. Here’s a statement from one of my favorite blogs, Ask The Farmer’s, article about the needs and risks of antibiotics:
|
“Farmers understand the gravity of the antibiotic resistance bacteria problem. And even though there has been no link between what we do on the farm and antibiotic resistance, we are still moving to the forefront of the issue and demonstrate to consumers we are doing the right thing. On the other hand, we need to care for our [animals]. When our [livestock] get sick, we need to help them. It’s our responsibility.” |
For these reasons, I personally do not purchase any products labeled with marketing gimmicks such as, “Raised Without the Use of Antibiotics,” or “Free of Antibiotics.” The truth is that even products coming from animals that have received antibiotic treatment can still be labeled as “Antibiotic Free” if enough time passed between receiving the injections and being slaughtered. Farms that operate “Without the Use of Antibiotics” may still administer antibiotics to sick animals, then just remove those from the group, which in turn distresses them further.
|
Companies have gotten a lot of attention and no doubt boosted their sales by announcing that they will no longer sell meat from animals that were given antibiotics. However, the majority of people that bounce at these kinds of slogans are usually not educated in the uses of antibiotics or even versed in the threat of bacterial resistance (discussed below). Of course the choice is up to you, but people should not be making uninformed buying decisions based off of illegitimate fears… especially when those products may present an even greater threat to food safety and animal welfare.
|
Photo from http://safer-america.com/deceptive-food-labeling/
|
Withdrawal Periods
If an animal receives any antibiotics, and often even medications outside the realm of antibiotics, they must wait a specified withdrawal period, which is an amount of time devoid of the medication to let it pass out of their system, before they are slaughtered or any products are obtained from them (such as milk).
Each type of antibiotic has been evaluated by the FDA to determine the accurate dosage (which is listed on the label) depending on weight and species, and then the withdrawal period needed for it to be naturally removed.
Quality Control
Individual farms often screen for any antimicrobial residue in their products before they are shipped off for processing or sale. Dairies are probably the most well-known for this because a single drop of milk with traces of antibiotic residue can taint an entire container of milk, meaning it would all have to be dumped: profits literally down the drain. Failure to do this could mean an even larger supply of milk would have to be thrown out when the milk truck, which does an additional screening at the request of various regulatory agencies (most working with or under the FDA), tanks it for transport.
The USDA also plays a very active role in the fight against antibiotic residues: every slaughterhouse in America is subject to random inspections where meat is sampled for both residues and pathogens (pathogens could be a result of not treating diseases with antibiotics—it’s a two way street).
In processing plants, livestock are also screened for use of antibiotics both before and after death. Methods of detecting abnormalities while the animals are still alive include checking for knots at possible injection sites and making sure that the animal is eating, drinking, and behaving normally. Many smaller processing plants actually converse with the breeder to discuss antibiotic usage and the importance of removing residues and avoiding bacterial resistance. Plant workers have found that producers are often compliant with the value of public welfare.
After death, blood trials and chemical evaluations of the meat (often done with swab tests) are a more accurate assessment of antimicrobial presence. Because cuts of meat are kept separate and many plants have systems allowing them to know what pieces came from which animals, cross contamination is less likely than in milk, but is still kept in consideration.
If an animal receives any antibiotics, and often even medications outside the realm of antibiotics, they must wait a specified withdrawal period, which is an amount of time devoid of the medication to let it pass out of their system, before they are slaughtered or any products are obtained from them (such as milk).
Each type of antibiotic has been evaluated by the FDA to determine the accurate dosage (which is listed on the label) depending on weight and species, and then the withdrawal period needed for it to be naturally removed.
Quality Control
Individual farms often screen for any antimicrobial residue in their products before they are shipped off for processing or sale. Dairies are probably the most well-known for this because a single drop of milk with traces of antibiotic residue can taint an entire container of milk, meaning it would all have to be dumped: profits literally down the drain. Failure to do this could mean an even larger supply of milk would have to be thrown out when the milk truck, which does an additional screening at the request of various regulatory agencies (most working with or under the FDA), tanks it for transport.
The USDA also plays a very active role in the fight against antibiotic residues: every slaughterhouse in America is subject to random inspections where meat is sampled for both residues and pathogens (pathogens could be a result of not treating diseases with antibiotics—it’s a two way street).
In processing plants, livestock are also screened for use of antibiotics both before and after death. Methods of detecting abnormalities while the animals are still alive include checking for knots at possible injection sites and making sure that the animal is eating, drinking, and behaving normally. Many smaller processing plants actually converse with the breeder to discuss antibiotic usage and the importance of removing residues and avoiding bacterial resistance. Plant workers have found that producers are often compliant with the value of public welfare.
After death, blood trials and chemical evaluations of the meat (often done with swab tests) are a more accurate assessment of antimicrobial presence. Because cuts of meat are kept separate and many plants have systems allowing them to know what pieces came from which animals, cross contamination is less likely than in milk, but is still kept in consideration.
|
Bacterial Resistance
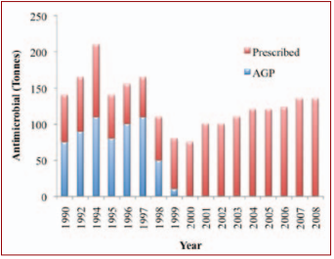
Due to concerns about bacterial resistance to antimicrobial drugs, starting in 1999, Denmark banned the use of AGP’s, or Antimicrobial Growth Promoters. This is much like what the FDA is attempting in American agriculture. By monitoring the trends of antibiotic use from 1990-2008, officials noticed an overall decrease in total antibiotic use, but the amount of antibiotics used to treat animal disease actually increased (see graph). Throughout this period, which also involved increased monitoring and awareness of antibiotic use in humans, bacterial resistance was measured. Researcher conclusions were not at all what they had expected to find: |
“While resistance in bacteria from livestock decreased, resistance in bacteria from humans remained the same or increased in almost every type of bacteria tested. In many cases, the increase in resistance to specific drugs was likely caused by increased use of that drug in human medicine.”
This means that reducing antibiotic use in livestock will not protect humans from bacteria that develop resistance to medications. Similar programs were enacted in Sweden and Norway, and the conclusions were the same.
In 2003, a program called Guidance 152 was instated by the FDA that lays out acceptable antibiotic usage in livestock as well as reaction plans in the case of resistant bacteria outbreaks. The FDA has denied or restricted many antibiotic types because of their high risk potential. This program has offered researchers unprecedented insight into resistance patterns which has resulted in improved public health recommendations.
Bacterial resistance is a very real threat, but researchers, doctors, veterinarians, and livestock raisers have all addressed the problem proactively. Millions of dollars and countless hours have been invested into assessing the risks of antibiotic use in animals and people. Scientists are more confident than ever that, if a problem was to arise, data obtained from previous antibiotic usage would allow them to keep people out of harm's way.
Sources
Jeong, Sang-Hee, Daejin Kang, Myung-Woon Lim, Chang Soo Kang, and Ha Jung Sung. "Risk Assessment of Growth Hormones
and Antimicrobial Residues in Meat."Toxicological Research. The Korean Society of Toxicology, Dec. 2010. Web. 02 Apr.
2017.
Masztis, P. S. "Antibiotic Residue Testing in a Beef Slaughterhouse." The Canadian Veterinary Journal. U.S. National Library of
Medicine, Aug. 1984. Web. 02 Apr. 2017.
Mountjoy, Brittany. "Fact Sheet: FDA's Approval Process for Food Animal Antibiotics."FoodInsight.org. International Center of
Excellence in Food Risk Communication, 2 Oct. 2014. Web. 02 Apr. 2017.
NC Meat Mom. "McDonalds and Costco Make Headlines ; Farmers and Processors Make Safe Food." NC Meat Mom. WordPress,
08 Mar. 2015. Web. 02 Apr. 2017.
Patsche, Wanda. "What You Really Need To Know About Antibiotics In Livestock." Ask The Farmers. Ask the Farmers, 21 Sept.
2015. Web. 02 Apr. 2017.
Rushing, John E., PhD, and D.P. Wesen, PhD. "Preventing Antibiotic Residues in Milk."FBNS. NCSU Department of Food Science, n.d. Web. 2 Apr. 2017.
Shlaes, David M., and Steven J. Projan. "Antimicrobial Resistance Versus the Discovery and Development of New
Antimicrobials." Antimicrobial Drug Resistance (2009): 43-50.Purdue Extension. Purdue University. Web. 2 Apr. 2017.
This means that reducing antibiotic use in livestock will not protect humans from bacteria that develop resistance to medications. Similar programs were enacted in Sweden and Norway, and the conclusions were the same.
In 2003, a program called Guidance 152 was instated by the FDA that lays out acceptable antibiotic usage in livestock as well as reaction plans in the case of resistant bacteria outbreaks. The FDA has denied or restricted many antibiotic types because of their high risk potential. This program has offered researchers unprecedented insight into resistance patterns which has resulted in improved public health recommendations.
Bacterial resistance is a very real threat, but researchers, doctors, veterinarians, and livestock raisers have all addressed the problem proactively. Millions of dollars and countless hours have been invested into assessing the risks of antibiotic use in animals and people. Scientists are more confident than ever that, if a problem was to arise, data obtained from previous antibiotic usage would allow them to keep people out of harm's way.
Sources
Jeong, Sang-Hee, Daejin Kang, Myung-Woon Lim, Chang Soo Kang, and Ha Jung Sung. "Risk Assessment of Growth Hormones
and Antimicrobial Residues in Meat."Toxicological Research. The Korean Society of Toxicology, Dec. 2010. Web. 02 Apr.
2017.
Masztis, P. S. "Antibiotic Residue Testing in a Beef Slaughterhouse." The Canadian Veterinary Journal. U.S. National Library of
Medicine, Aug. 1984. Web. 02 Apr. 2017.
Mountjoy, Brittany. "Fact Sheet: FDA's Approval Process for Food Animal Antibiotics."FoodInsight.org. International Center of
Excellence in Food Risk Communication, 2 Oct. 2014. Web. 02 Apr. 2017.
NC Meat Mom. "McDonalds and Costco Make Headlines ; Farmers and Processors Make Safe Food." NC Meat Mom. WordPress,
08 Mar. 2015. Web. 02 Apr. 2017.
Patsche, Wanda. "What You Really Need To Know About Antibiotics In Livestock." Ask The Farmers. Ask the Farmers, 21 Sept.
2015. Web. 02 Apr. 2017.
Rushing, John E., PhD, and D.P. Wesen, PhD. "Preventing Antibiotic Residues in Milk."FBNS. NCSU Department of Food Science, n.d. Web. 2 Apr. 2017.
Shlaes, David M., and Steven J. Projan. "Antimicrobial Resistance Versus the Discovery and Development of New
Antimicrobials." Antimicrobial Drug Resistance (2009): 43-50.Purdue Extension. Purdue University. Web. 2 Apr. 2017.
Share this: